Thyroid cancer is increasing faster than any other type of cancer in the United States, and similar trends are emerging in other parts of the world. Experts say the rise is linked both to improved detection methods and lifestyle factors such as obesity.
The thyroid, a small gland at the base of the neck, produces hormones that regulate metabolism, heart rate, and body temperature. Cancer occurs when thyroid cells grow uncontrollably, forming a tumour that can invade nearby tissues or spread to other organs. While most thyroid cancers are treatable, the rapid increase in cases has raised concern among medical professionals.
Data from the U.S. Surveillance, Epidemiology, and End Results (SEER) program shows that between 1980 and 2016, thyroid cancer incidence more than tripled, rising from 2.39 to 7.54 per 100,000 men and from 6.15 to 21.28 per 100,000 women. Endocrine surgeon Sanziana Roman of UCSF notes that thyroid cancer is one of the few cancers consistently rising despite medical advances.
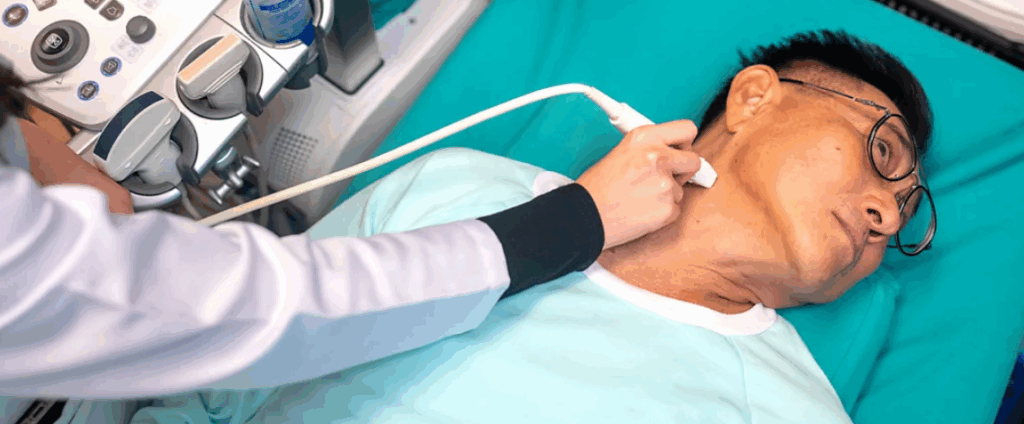
Part of the increase is attributed to better diagnosis. In the 1980s, thyroid ultrasonography allowed doctors to detect very small tumours that would previously have gone unnoticed. The 1990s brought fine needle aspiration biopsies to confirm cancer in suspicious nodules. These techniques led to a surge in diagnoses of small papillary thyroid cancers, which are slow-growing and rarely fatal. South Korea saw a similar pattern when a national screening programme caused thyroid cancer rates to soar before declining once screenings were scaled back.
Despite improvements in early detection, studies indicate that overdiagnosis does not explain the entire rise. Research from California found that both incidence and mortality increased from 2000 to 2017, even for larger or more advanced tumours. Similarly, SEER data suggests that while overall rates have stabilized in the U.S., deaths from thyroid cancer remain steady at around 0.5 per 100,000.
Experts point to obesity as a likely contributor. High body mass index (BMI) is associated with a 50% higher risk of thyroid cancer and more aggressive tumour features, including larger size and mutations that promote spread. Obesity-related factors such as inflammation, insulin resistance, and elevated thyroid-stimulating hormone may all play a role.
Environmental factors are also under investigation. Endocrine-disrupting chemicals found in cookware, packaging, personal care products, and firefighting foam may affect thyroid function, though evidence is mixed. Trace elements like zinc, cadmium, and vanadium, particularly in volcanic regions or island nations, have also been linked to higher thyroid cancer rates, but robust studies are limited.
Cari Kitahara, an epidemiologist at the National Cancer Institute, emphasizes that rising thyroid cancer rates are likely the result of multiple factors: improved detection, obesity, and environmental exposures. Advances in clinical practice now limit unnecessary surgery and radioactive iodine treatment, focusing instead on aggressive cancers while employing partial removal or active surveillance for smaller tumours.
The combination of heightened diagnosis, lifestyle changes, and possible environmental contributors suggests that thyroid cancer will remain a public health focus in coming years.